In the poignant journey towards end-of-life, every individual deserves care that’s as physically comfortable as it is emotionally nurturing. The U.S government’s resource ‘Providing Care and Comfort at the End of Life‘ delivers some remarkable insights on the subject, discussing the concept of care applicable during the final stages of life depending on an individual’s unique preferences. The essence of optimal care lies in addressing four critical aspects: physical comfort, mental and emotional needs, spiritual aspirations, and practical tasks. Physical comfort includes managing pain, breathing difficulties, skin irritations, and fatigue, among others – often requiring medication or environmental modifications.
However, a holistic approach to end-of-life care goes beyond just meeting the physical requirements; it must incorporate attention to mental and emotional states, ease fears, and provide access to counselling if necessary. Moreover, end-of-life care develops a supportive paradigm for the family or loved ones, recognizing their needs and emotional upheaval as they journey alongside.
Understanding End-of-Life Care
Definition and significance of end-of-life care
End-of-life care refers to the support and medical service provided to individuals nearing their death. The duration of this type of care can differ from a couple of days to even several weeks or months, depending on an individual’s health status. Its importance lies in the ability to provide quality care, comfort, and support during the last stages of life, ensuring that your last days are as peaceful and fulfilling as possible.
The dying person’s preference
People have diverse thoughts, beliefs, and preferences when it comes to the end of their lives. Some prefer to die in the comfort of their homes surrounded by loved ones, while others prefer the advanced tools and services available in a hospital or care facility. The dying person’s preference plays a significant role in dictating the nature of their end-of-life journey.
The importance of a holistic approach
End-of-life care isn’t just focused on physical comfort or medical needs. It encompasses a holistic approach that goes above and beyond to cater to mental, emotional, spiritual aspects, and practical needs such as legal and financial matters. The goal is to exceed the care standards by ensuring that all areas of the dying person’s needs are met, providing them with comprehensive support.
Components of Optimal End-of-Life Care
Physical comfort
The maintenance of physical comfort forms a critical part of end-of-life care. Techniques like prescribing medication for pain, addressing breathing issues, and mitigating skin irritations provide the patient with the comfort they need at this time.
Mental and emotional needs
Paying attention to mental and emotional needs is equally important. This can include managing feelings of depression and anxiety and addressing any other fears or concerns the dying person may have. Counseling services or medication may be recommended to help ease emotional distress.
Spiritual needs
Some individuals find comfort and peace in spiritual beliefs and practices towards the end of their life. Therefore, honoring, and incorporating these spiritual elements into the care plan plays a vital role in optimizing end-of-life care
Practical tasks
Practical tasks such as making financial plans, organizing personal affairs, ensuring legal matters are set, and planning the last respects are crucial. Such tasks offer the dying person peace of mind, knowing that their affairs are in order.
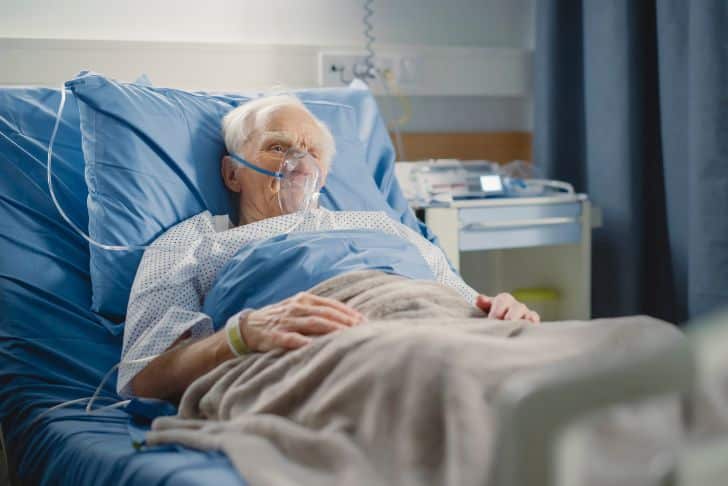
Managing Physical Comfort Towards the End of Life
Dealing with pain
Pain management is a critical component of creating physical comfort. Medical professionals may prescribe pain medication or recommend various techniques to alleviate pain, such as massage or physical therapy.
Addressing breathing problems
Breathing problems can be a significant issue towards the end of life. To address these problems, health care providers may offer treatments or tools to aid respiration, such as oxygen masks or specific exercises.
Taking care of skin irritations
Skin can become sensitive and susceptible to irritations near the end of life. Caregivers can alleviate these discomforts by keeping the skin clean, applying topical remedies, and repositioning the patient regularly.
Managing digestive problems
Digestive problems such as constipation or loss of appetite can cause discomfort. Health care professionals can advise on appropriate diet changes, medication, or strategies to alleviate these problems and maintain physical comfort.
Addressing temperature sensitivity and fatigue
The body might become more sensitive to temperature changes and more prone to fatigue. Ensuring a comfortable environment by controlling room temperature and allowing for ample rest can add tremendous comfort.
Involvement of medication, environmental changes, and comfort aids in physical comfort
A holistic approach considers all possible solutions to optimize physical comfort, from medication and environmental changes to the use of comfort aids like cushions, blankets, and adjustable beds.
Attending to Mental and Emotional Needs
Managing depression
End-of-life can often be accompanied by feelings of sadness or depression. Access to mental health professionals for counseling or medication can provide relief during this challenging time.
Coping with anxiety
Anxiety can be common, given the circumstances. Various coping strategies and therapeutic interventions, such as mindfulness techniques or talk therapy, can be beneficial in reducing anxiety.
Aiding in dealing with fears or concerns
Having honest conversations about their fears and concerns and offering reassurances where possible can alleviate the individual’s distress. Therapeutic conversations with a counselor can also be incredibly helpful.
The role of counseling and medication
Counseling and medication can play a role in managing mental and emotional distress. These provide a helpful platform for expressing feelings and gaining insight while maintaining emotional stability.

Catering to Spiritual Needs
Incorporating religious beliefs and practices
For those who hold a strong religious faith, incorporating religious beliefs and practices into their care can offer immense comfort and peace.
Providing a sense of peace and acceptance
Spiritual guidance can help individuals find peace and acceptance towards the end of their life, enabling them to come to terms with their mortality and find comfort in their beliefs or philosophy.
Spiritual guidance and counseling
Chaplains or spiritual counselors can provide valuable guidance and support during this time, helping to meet the spiritual needs of the dying individual.
Addressing Practical Tasks
Making financial plans
Financial planning towards the end of life helps ensure that all affairs are in order and can ease significant stress for both the dying person and their loved ones.
Organizing personal affairs
Whether it’s organizing documents, passing on heirlooms or saying goodbyes, keeping personal affairs in order can offer a sense of control and fulfillment during this time.
Ensuring legal matters are in place
Legal matters such as creating or updating a will, assigning an executor, and outlining care preferences ensure that the dying person’s wishes are respected and followed.
Planning the last rites
The planning of last rites or funeral arrangements is an essential aspect of end-of-life care, respecting the dying person’s wishes and providing closure for the loved ones left behind.

The Role of Health Care Providers
Understanding the responsibilities of health care providers in end-of-life care
Health care providers are responsible for ensuring the dying person’s comfort, coordinating the necessary care services, implementing a care plan, and offering support to loved ones.
The importance of communication in providing optimal care
Transparent, empathetic, and open communication between health care providers, the dying individual, and their family is vital in providing optimal care, understanding needs and preferences, and finding the most fitting care solutions.
Creating a care plan
Creating a care plan helps to guide the end-of-life care process, outlining the individual’s health status, care preferences and options, and deciding on what interventions are needed.
Support for the Support System
Why end-of-life care also involves the family or loved ones
End-of-life isn’t just about the dying person. It also deeply affects the people around them. Thus, end-of-life care extends to the support system, including family, friends and any other loved ones involved in the care process, providing them with the necessary help and support.
Types of support needed by loved ones
Loved ones might need various types of support, from understanding how to care for the dying individual to undergoing their grief journey. By offering emotional support, education, and resources, caregivers can help them navigate this difficult time.
Resources for family and friends
Many resources are available for family and friends to help them during this period. From psychological resources, such as counseling services, to practical newsletters on managing the care process, various resources can provide the needed support.
The Importance of Advanced Care Planning
What is advanced care planning
Advanced care planning involves making decisions about the types of care and treatments the individual might want towards the end of their life. It ensures that the person’s preferences are respected, should they be unable to communicate their decisions in the future.
The role of advanced care planning in end-of-life care
Advanced care planning plays a crucial role in end-of-life care. It sets clear guidelines for health care providers and loved ones to follow, ensuring that the individual’s health care desires are respected, even if they can’t express them.
Benefits of advanced care planning
Advanced care planning benefits both the dying person and their loved ones. It provides a clear course of action, reduces stress and uncertainty, and offers peace of mind knowing that the dying person’s wishes will be honored.
End-of-Life Care Across Different Settings
End-of-life care at home
Some individuals prefer receiving end-of-life care in the familiarity and comfort of their own home. Here, personal care and medical intervention can be adjusted to the home setting.
End-of-life care in a hospital setting
Hospital care is another option, where the patient has access to physical, mental, and emotional support, as well as advanced medical treatments and monitoring.
End-of-life care in a hospice or care facility
A hospice or care facility can provide a middle ground between a hospital and home setting. These facilities offer skilled care, including pain and symptom management, while also providing comfort.
Comparing different settings for end-of-life care
There’s no one-size-fits-all answer to the best setting for end-of-life care. The choice depends on individual preferences, medical requirements, family support systems, financial resources, and other factors. Each setting has its unique advantages to consider.
End-of-life care is about ensuring comfort, dignity, and quality of life in the final stages. By understanding and addressing the diverse needs of the dying person, we can create a supportive and compassionate environment for them and their loved ones.
